Your gift is 100% tax deductible.
New AI Tool Improves the Accuracy of a Breast Cancer Prognosis
Artificial intelligence (AI) tumor analyses help pathologists predict the future course of a woman's breast cancer.
The Challenge
All breast cancers aren't the same. A specialized doctor called a pathologist learns about each person's breast cancer by carefully evaluating how a sample of tumor cells look under a microscope. They're assessing how different the cells look from normal breast cells, the cells' arrangement, and the number of dividing cancer cells. Together, these characteristics help the pathologist determine how likely it is that the cancer will grow and spread.
Currently, the cancer's grade is combined with other features of the tumor, including the TNM stage and the ER/PR/HER2 hormone status, to determine the diagnosis and doctor's best estimate of the cancer's prognosis. The prognosis is a prediction about the patient's expected outcome—the likelihood of recovery from, or recurrence, of the cancer. The patient's oncologist uses this information to talk with the patient about the best course of treatment.
Recent research has shown that evaluating the noncancerous elements in the tumor microenvironment also supplies helpful information about how the cancer might progress. That microenvironment outside tumor cells includes immune cells and other structures that can either inhibit or promote cancer growth and provide shape around a tumor.
While there are some excellent, experienced pathologists who specialize in breast cancer, analyzing the microscopic cancerous and noncancerous cells with the human eye is neither expedient nor efficient. A modern innovation that supports and improves the pathologist's task is digital pathology. This process uses specialized computer scanners and software to convert glass slides of tissue samples into high-resolution digital images that pathologists view on a computer monitor. Just like photos, digital images can be more quickly shared with others via the internet and without the concern of damaging the slides.
The Research
A group of Northwestern University and American Cancer Society researchers recently developed a breast cancer prognosis score using an artificial intelligence (AI) analysis of breast cancer tissue. This research, published in the scientific journal Nature Medicine, was particularly novel because it incorporated information about noncancerous cells surrounding the tumor into the score.
The overall goal of the work was to improve the accuracy, reproducibility, and efficiency of a patient's prognosis. Using the newly identified elements of the score along with other clinical data already collected in routine practice allows pathologists and doctors to use the new prognosis score to better predict the prognosis of the patient, and therefore, decide if the patient would benefit from chemotherapy or other additional aggressive treatment.
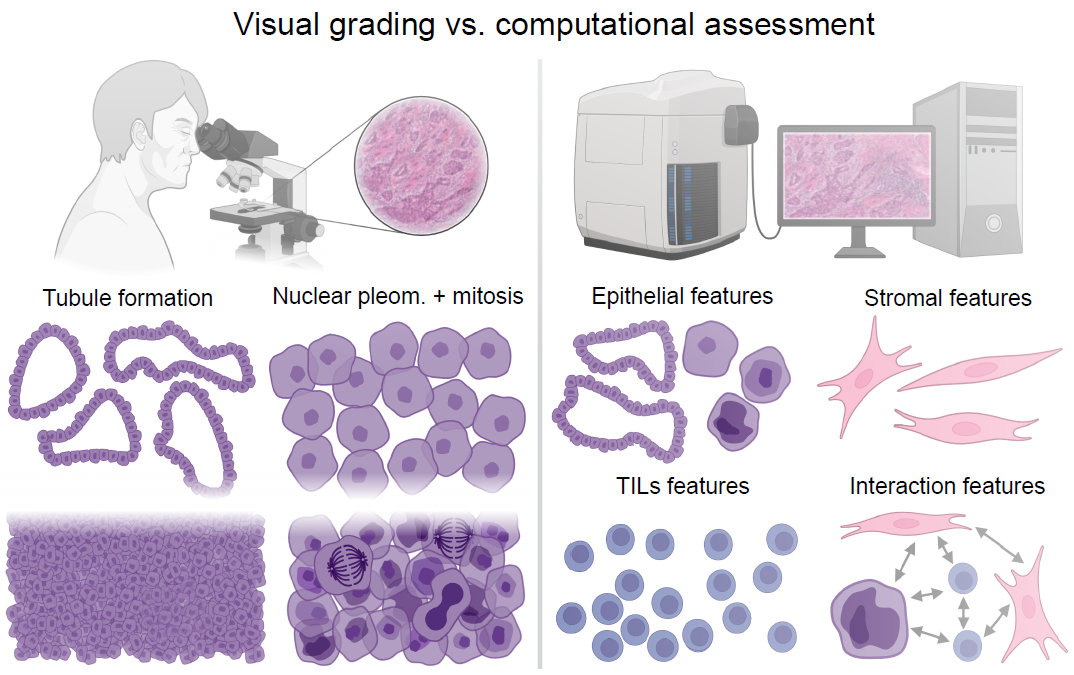
This figure was created using BioRender. The faded white area of the image on the left demonstrates that there are more steps than shown.
The left side of the above graphic shows the qualitative steps a pathologist uses to visually determine a cancer’s grade: Use a microscope to see how cancer cells appear and predict how they will grow to provide a grade to help the oncologist discuss treatment options with the patient.
The right side of the above graphic shows the quantitative steps the AI model uses to determine the cancer's grade. To start the process, the computer monitor in the graphic demonstrates the digital image of the slide with breast tissue. The assessment of this whole-slide image (WSI) uses advanced deep-learning computer vision to identify different cells and examine the cells' relationship to one another. The result is a more comprehensive evaluation of the entire area around a cancer than what is currently evaluated. Pathologists who use these specialized methods of artificial intelligence and integrated, computerized assessments (known as machine learning) are part of a brand-new discipline called computational pathology.
The new AI-enhanced breast cancer prognosis score, called HiPS, analyzes 26 different features of a patient's breast tissue to generate the score. The computer program that calculates the score does "interpretable scoring," meaning that it also "explains" to the pathologist which exact features are important for survival. Women with breast cancer are categorized as high risk if their cancer is likely to progress and possibly lead to death. Oncologists prescribe more aggressive treatments, like chemotherapy for high-risk patients. Patients who have a low risk of dying from breast cancer can often avoid these aggressive treatments, which have many difficult side effects.
HiPS was developed using data from sample tissue of 3,177 breast cancer patients who were part of the large prospective cohort from the ACS Cancer Prevention Study-II (CPS-II), and it was validated using data from ACS CPS-3, along with two other non-ACS related cohorts.
The dataset from CPS-II includes women diagnosed in hundreds of US healthcare facilities ranging from large academic cancer centers to rural facilities from over 614 US counties in 48 states. CPS-II data also included a wide representation of breast cancers in terms of size and aggressiveness. This diversity allowed the AI model to capture the true spectrum of disease in the US and improve its accuracy across breast cancers with different characteristics.
Another valuable feature of the ACS studies is that we have more than just the cancer tissue samples that other tissue databases provide—we also have decades of follow-up data from patients. This long-term information provides many valuable insights including the date a patient dies and what they die of. The ACS CPS-II resources were what made this high-impact work possible.
The collaborative study relied on the computational pathologists Mohamed Amgad, MS, PhD, and Lee Cooper, PhD, from Northwestern University to develop the AI algorithm. Scientists from the American Cancer Society (ACS) provided expertise on breast cancer epidemiology and clinical outcomes for the study. ACS co-authors included James Hodge, JD, MPH, Clara Bodelon, PhD, MS, and Lauren Teras, PhD.
Next, researchers will need to evaluate the HiPS model using data from clinical trials before it can be used in clinical practice.
Why It Matters
The HiPS AI model has the potential to:
- Improve current prognosis methods. When the HiPS score is approved for clinical practice, pathologists may be able to recategorize some women who are currently classified as high-risk (and thus, recommended aggressive treatment with chemotherapy) into a lower-risk category. That means that more women may be able to avoid chemotherapy or other intense and long treatments that often have many challenging side effects.
- Increase the number of patients who receive a more evidenced-based prognosis. The internet allows a quick transfer of HiPS information across long distances. As digital technology continues to be more widely available, HiPS evaluations can follow, regardless of where patients are or their access to a pathologist specialized in breast cancer.
- Related resources
- For researchers
Glowing "Fingerprint" from a Blood Test May Find Ovarian Cancer Early For more about Machine Learning
American Cancer Society and Yosemite Award $6 Million in Research Grants to Innovative Cancer Scientists (Press release) For more about funding AI Cancer Research



